Cervical cancer
What is cervical cancer?
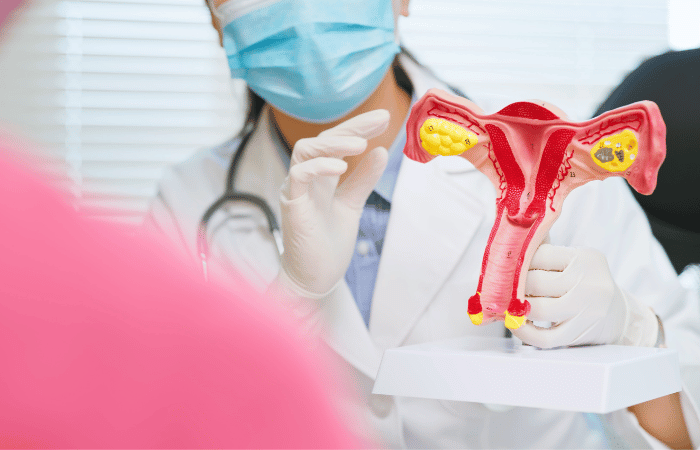
What is cervical cancer?
Cervical cancer happens when cells change in a woman’s cervix, which connects her uterus with her vagina. This cancer can affect the deeper tissues of her cervix and may spread to other parts of her body (metastasize), often the lungs, liver, bladder, vagina, and rectum.
Most cases of cervical cancer are caused by infection with human papillomavirus (HPV), which is preventable with a vaccine.
Cervical cancer grows slowly, so there’s usually time to find and treat it before it causes serious problems. It kills fewer and fewer women each year, thanks to improved screening through Pap tests.
Women 35 to 44 years old are most likely to get it. More than 15% of new cases are in women over age 65, however, especially those who haven’t been getting regular screenings.
Cervical cancer is a type of cancer that starts in the cervix. The cervix is a hollow cylinder that connects the lower part of a woman’s uterus to her vagina. Most cervical cancers begin in cells on the surface of the cervix.
The cervix is made of two parts and is covered with two different types of cells.
- The endocervix is the opening of the cervix that leads into the uterus. It is covered with glandular cells.
- The exocervix (or ectocervix) is the outer part of the cervix that can be seen by the doctor during a speculum exam. It is covered in squamous cells.
The place where these two cell types meet in the cervix is called the transformation zone. The exact location of the transformation zone changes as you get older and if you give birth. Most cervical cancers begin in the cells in the transformation zone.
 Pre-cancer of the cervix
Pre-cancer of the cervix
Cells in the transformation zone do not suddenly change into cancer. Instead, the normal cells of the cervix first gradually develop abnormal changes that are called pre-cancerous. Doctors use several terms to describe these pre-cancerous changes, including cervical intraepithelial neoplasia (CIN), squamous intraepithelial lesion (SIL), and dysplasia.
When the pre-cancers are checked in the lab, they are graded on a scale of 1 to 3 based on how much of the cervical tissue looks abnormal.
- In CIN1 (also called mild dysplasia or low grade SIL), not much of the tissue looks abnormal, and it is considered the least serious cervical pre-cancer.
- In CIN2 or CIN3 (also called moderate/severe dysplasia or high-grade SIL) more of the tissue looks abnormal; high-grade SIL is the most serious pre-cancer.
Although cervical cancers start from cells with pre-cancerous changes (pre-cancers), only some of the women with pre-cancers of the cervix will develop cancer. For most women, pre-cancerous cells will go away without any treatment. But, in some women pre-cancers turn into true (invasive) cancers. Treating cervical pre-cancers can prevent almost all cervical cancers.
Pre-cancerous changes can be detected by the Pap test and treated to prevent cancer from developing. See Can Cervical Cancer Be Prevented? Pre-cancerous changes found on your Pap test and specific types of treatment for pre-cancers are discussed in The Pap Test and Work-up of Abnormal Pap Test Results.
Types of cervical cancer
Cervical cancers and cervical pre-cancers are classified by how they look in the lab s with a microscope. The main types of cervical cancers are squamous cell carcinoma and adenocarcinoma.
- Most (up to 9 out of 10) cervical cancers are squamous cell carcinomas. These cancers develop from cells in the exocervix. Squamous cell carcinomas most often begin in the transformation zone (where the exocervix joins the endocervix).
- Most of the other cervical cancers are adenocarcinomas. Adenocarcinomas are cancers that develop from glandular cells. Cervical adenocarcinoma develops from the mucus-producing gland cells of the endocervix.
- Less commonly, cervical cancers have features of both squamous cell carcinomas and adenocarcinomas. These are called adenosquamous carcinomas or mixed carcinomas.
Although almost all cervical cancers are either squamous cell carcinomas or adenocarcinomas, other types of cancer also can develop in the cervix. These other types, such as melanoma, sarcoma, and lymphoma, occur more commonly in other parts of the body.

What are the risk factors of cervical cancer?
Almost all cervical cancers are caused by human papillomavirus (HPV), a common virus that can be passed from one person to another during sex. There are many types of HPV. Some HPV types can cause changes on a woman’s cervix that can lead to cervical cancer over time, while other types can cause genital or skin warts.
HPV is so common that most people get it at some time in their lives. HPV usually causes no symptoms so you can’t tell that you have it. For most women, HPV will go away on its own; however, if it does not, there is a chance that over time it may cause cervical cancer.
Other things can increase your risk of cervical cancer—
- Having HIV (the virus that causes AIDS) or another condition that makes it hard for your body to fight off health problems.
- Smoking.
- Using birth control pills for a long time (five or more years).
- Having given birth to three or more children.
- Having several sexual partners.
What are the causes of cervical cancer?
Cervical cancer begins when healthy cells in the cervix develop changes (mutations) in their DNA. A cell’s DNA contains the instructions that tell a cell what to do.
Healthy cells grow and multiply at a set rate, eventually dying at a set time. The mutations tell the cells to grow and multiply out of control, and they don’t die. The accumulating abnormal cells form a mass (tumor). Cancer cells invade nearby tissues and can break off from a tumor to spread (metastasize) elsewhere in the body.
It isn’t clear what causes cervical cancer, but it’s certain that HPV plays a role. HPV is very common, and most people with the virus never develop cancer. This means other factors — such as your environment or your lifestyle choices — also determine whether you’ll develop cervical cancer.
Cervical cancer treatment
Cervical cancer is very treatable if you catch it early. The four main treatments are:
Sometimes these treatments are combined to make them more effective.
Surgery
The purpose of surgery is to remove as much of the cancer as possible. Sometimes the doctor can remove just the area of the cervix that contains cancer cells. For cancer that’s more widespread, surgery may involve removing the cervix and other organs in the pelvis.
Radiation therapy
Radiation kills cancer cells using high-energy X-ray beams. It can be delivered through a machine outside the body. It can also be delivered from inside the body using a metal tube placed in the uterus or vagina.
Chemotherapy
Chemotherapy uses drugs to kill cancer cells throughout the body. Doctors give this treatment in cycles. You’ll get chemo for a period of time. You’ll then stop the treatment to give your body time to recover.
Targeted therapy
Bevacizumab (Avastin) is a newer drug that works in a different way from chemotherapy and radiation. It blocks the growth of new blood vessels that help the cancer grow and survive. This drug is often given together with chemotherapy.
If your doctor discovers precancerous cells in your cervix they can be treated. See what methods stop these cells from turning into cancer.
What are the stages of cervical cancer?
After you’ve been diagnosed, your doctor will assign your cancer a stage. The stage tells whether the cancer has spread, and if so, how far it’s spread. Staging your cancer can help your doctor find the right treatment for you.Cervical cancer has four stages:
- Stage 1: The cancer is small. It may have spread to the lymph nodes. It hasn’t spread to other parts of your body.
- Stage 2: The cancer is larger. It may have spread outside of the uterus and cervix or to the lymph nodes. It still hasn’t reached other parts of your body.
- Stage 3: The cancer has spread to the lower part of the vagina or to the pelvis. It may be blocking the ureters, the tubes that carry urine from the kidneys to the bladder. It hasn’t spread to other parts of your body.
- Stage 4: The cancer may have spread outside of the pelvis to organs like your lungs, bones, or liver.
Diagnosis of cervical cancer
Screening tests can help detect cervical cancer and precancerous cells that may one day develop into cervical cancer. Most guidelines suggest beginning screening for cervical cancer and precancerous changes at age 21.
Screening tests include:
- Pap test. During a Pap test, your doctor scrapes and brushes cells from your cervix, which are then examined in a lab for abnormalities. A Pap test can detect abnormal cells in the cervix, including cancer cells and cells that show changes that increase the risk of cervical cancer.
- HPVDNA test. The HPV DNA test involves testing cells collected from the cervix for infection with any of the types of HPV that are most likely to lead to cervical cancer.
Discuss your cervical cancer screening options with your doctor.
If cervical cancer is suspected, your doctor is likely to start with a thorough examination of your cervix. A special magnifying instrument (colposcope) is used to check for abnormal cells.
During the colposcopic examination, your doctor is likely to take a sample of cervical cells (biopsy) for laboratory testing. To obtain tissue, your doctor may use:
- Punch biopsy, which involves using a sharp tool to pinch off small samples of cervical tissue.
- Endocervical curettage, which uses a small, spoon-shaped instrument (curet) or a thin brush to scrape a tissue sample from the cervix.
If the punch biopsy or endocervical curettage is worrisome, your doctor may perform one of the following tests:
- Electrical wire loop, which uses a thin, low-voltage electrified wire to obtain a small tissue sample. Generally this is done under local anesthesia in the office.
- Cone biopsy (conization), which is a procedure that allows your doctor to obtain deeper layers of cervical cells for laboratory testing. A cone biopsy may be done in a hospital under general anesthesia.
Prevention of cervical cancer
To reduce your risk of cervical cancer:
- Ask your doctor about the HPV vaccine. Receiving a vaccination to prevent HPV infection may reduce your risk of cervical cancer and other HPV-related cancers. Ask your doctor whether an HPV vaccine is appropriate for you.
- Have routine Pap tests. Pap tests can detect precancerous conditions of the cervix, so they can be monitored or treated in order to prevent cervical cancer. Most medical organizations suggest beginning routine Pap tests at age 21 and repeating them every few years.
- Practice safe sex. Reduce your risk of cervical cancer by taking measures to prevent sexually transmitted infections, such as using a condom every time you have sex and limiting the number of sexual partners you have.
- Don’t smoke. If you don’t smoke, don’t start. If you do smoke, talk to your doctor about strategies to help you quit.
For details on cervical cancer treatment and second opinion, do call us at +96 1588 1588 or write to info@cancerfax.com.
- Comments Closed
- July 28th, 2020
 Pre-cancer of the cervix
Pre-cancer of the cervix








Privacy Overview